Pulmonary actinomycosis: cytomorphological features
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Accepted: 22 September 2021
Authors
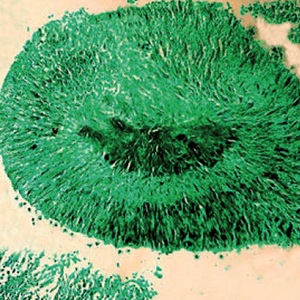
Pulmonary actinomycosis is an uncommon infectious disease. Although the gold standard for diagnosis is histological examination with bacterial culture of lung tissue, cytology samples offer a fast and low-cost alternate diagnostic procedure. The cytology literature on this topic is limited to mostly case reports. Therefore, the aim of this study was to review cytological material in a series of patients with a diagnosis of pulmonary actinomycosis to characterize the main cytomorphological findings. Different cytological respiratory samples including sputum smears, bronchoalveolar lavages (BALs), transthoracic or endobronchial fine needle aspiration cytology (FNAC) and cell block preparations were used for retrospective examination. For all cases patient age, gender, symptoms, and radiological chest findings were recorded. A total of 26 cytological respiratory samples (14 sputum smears, 9 FNAC, two BALs) including direct smears and 6 cell blocks from 9 patients were examined. In sputum smears the most remarkable findings were the presence of dark cotton ball masses with projections like spider legs and/or mouse tails (75% of the samples). Sulfur granules were observed in 4 (40%) of the sputum smears and within FNAC cases. Various respiratory cytology samples including sputum smears, FNAC and BALs can reveal cytomorphological findings diagnostic of pulmonary actinomycosis. Characteristic cytological findings compatible with a diagnosis of this infection include cotton ball masses and less frequently sulfur granules.
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






