Intermittent abdominal pressure ventilation: feasibility and efficacy in neuromuscular disease. A case report
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Authors
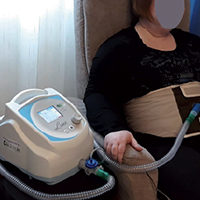
The standard treatment for patients with neuromuscular respiratory failure is non-invasive ventilation (NIV) as non-invasive ventilation support-setting (NVS). NVS is administered through a nasal or face mask and/or mouthpiece with the potential to cause nasal ulcers, discomfort, and/or aesthetic issues, resulting in poor compliance. We reported the observation of a 45-year-old woman with limb-girdle muscular dystrophy (LGMD), secondary to Dysferlin deficiency, who was on NVS since 2017 for nocturnal hypoventilation. In 2018, despite nocturnal ventilation, due to weight gain and daytime hypoventilation, a nasal mask was introduced. We initiated daytime intermittent abdominal pressure ventilation (IAPV) to mitigate cosmetic problems, improving in pO2 and decreasing in pCO2 versus baseline (52>84 mmHg, 46>33 mmHg respectively) at 6 (85 mmHg, 42 mmHg) and 18 months (93 mmHg, 38 mmHg), respectively. IAPV was effective, safe, and well-tolerated in our patients who did not tolerate standard daytime NVS with the known interface.
Rights
The authors have obtained the written informed consent of the patient mentioned in the article to collect her data and share her photo. The corresponding author is in possession of the written informed consent.How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






